Pigmentation is one of the most common reasons that patients seek help from aesthetic practitioners.
Skin cells within the epidermis known as melanocytes produce melanin (pigmentation) which gives us the colour of our skin, it is also the way that your body protects itself from external damage, such as ultraviolet rays (UV). Melanin is created in the melanocyte cells when Tyrosinase (enzyme) converts Tyrosine (amino acid) into Dopa III. This process develops further when melanin moves to the keratinocyte cells within the epidermis.
All skin colours contain the same number of melanocytes however, individuals who originate from areas where UV rays are more intensive, naturally have a darker skin tone. This is due to the melanocytes which are more active, responding to sun exposure, this in turn produces more pigment. Pigmentation due to sun damage may not present as visible changes to the skin for 10 to 20 years post exposure.
Pigmentation is classified as a passive or inflammatory condition and is distinguished by the cause of pigmentation. Passive pigmentation is a result of hormonal fluctuations, usually found in the deeper layers of the skin it can also be more difficult to treat. Inflammatory pigmentation however is due to external influences, usually more superficial within the skins epidermis and is usually easier to treat.
Types of Pigmentation
- Ephelides (Freckles)
- Solar Lentigines (Age/Sunspots)
- Hyperpigmentation
- Melasma (Chloasma)
- Post Inflammatory Pigmentation (PIH)
Types of Pigmentation
Ephelides
This type of pigmentation is hereditary, melanocytes within the skin produce more pigmentation, which can be intensified by sun exposure. Pigmentation presents as small areas (freckles) which can merge into larger patches. Although ephelides can occur in any skin type, it is most prevalent in Fitzpatrick I skins.
Solar Lentigines
Also known as age or sunspots they usually present after the age of forty and are a direct consequence of sun exposure. Often seen more in lighter skin tones, although they occur in any skin colour. Solar Lentigines appear on areas of sun exposure, such as the face and hands and present as flat dark brown patches of pigmentation with well-defined boarders.
Hyperpigmentation
Hyperpigmentation is part of an inflammatory response to trauma and found upper layers of the epidermis. External influences such as trauma includes sun damage, overzealous extraction of pimples, comedones and milia, chemical burns and post procedures.
Melasmas
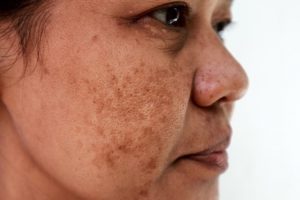
Melasmas present as mottled brown/grey flat patches of pigmentation that are more prominent in summer months as skin is exposed to ultraviolet rays. Melasmas are due to either hormonal imbalances, medications and medical conditions. Fluctuations in hormones can include pregnancy, birth control, hormonal replacement therapy or low testosterone levels.
Post Inflammatory Pigmentation
Post Inflammatory Pigmentation can occur in the epidermal and dermal layers of the skin and is due to an inflammatory response, which stimulates melanin production. PIH can present in any skins but is more common in Fitzpatrick III and above. A precursor to PIH may be other inflammatory conditions such as acne, eczema, psoriasis and systemic lupus erythematosus. Or it can be trauma such as previous aesthetic skin treatments or exposure to UV. Certain medications and allergies may also stimulate PIH. This condition usually resolves itself, however in some cases damage may be more permanent.
For many years now we have been aware of the damage ultraviolet B (UVB) exposure can cause and to prevent burning a high SPF is now used. However, it is only recently the photoaging damage produced in the dermal layer of skin by ultraviolet A (UVA) has become widely known.
The Difference Between UVA & UVB
UVA penetrates the deep dermal layer creating lasting DNA damage and premature ageing. UVA makes up 95% of the total UV rays and is present all year round, penetrating through glass and clouds. Dermal penetration affects blood and connective tissues, and skin shows signs of wrinkles due to a loss of elasticity. Melanin (pigmentation) within the cells of the epidermis is activated and there is an increase in oxidative stress. Oxidative stress within the skin is due to the damage caused by free radicals, which are generated by solar radiation. These free radicals produced by the sun are responsible for cell damage, blemishes and photoaging.
UVB rays penetrate the upper layer of the epidermis where melanin production is stimulated, and a suntan is produced. Cells within the epidermis reproduce faster and a thicker skin is created; both these reactions are a defensive mechanism to protect the skin and underlying tissues. Pigmentation areas and age spots occur on previously exposed areas to UV light, such as, face, chest, hands, arms and hands. To protect from UVB damage it is recommended an SPF of at least 30 is used. This translates to 30 times the UVB protection compared to no sunscreen being applied. It is important to remember that as well as direct sun rays, we can incur damage and sunburn from reflective surfaces such as snow, water and sand, and that UVA & UVB damage to skin cells can continue long after you have come out of the sun – approximately 3-4 hr.
Stress can also be a factor in pigmentation. Increases in the hormone cortisol produces inflammation within the skin, this inflammation combined with UV light creates oxidative stress (free radicals) resulting in pigmentation.
Treatments
The gold standard is to protect your skin from damaging UV rays. Following that, if there are areas of concern, then topical treatments such as skin peels or alkaline wash treatments along with effective skin care, formulated to supress melanin production are recommended. Other treatment options include cryotherapy, lasers and IPL. Unfortunately, some of the treatments and skin care available that target pigmentation may also create further trauma if not performed/used correctly.
Pigmentations vary in type, depth of colour, size and position within the skin, therefore a detailed consultation is required to physically assess your skin and consider any medical and lifestyle factors.
This consultation should include an examination with a skin analysis machine to identify if the pigmentation is passive, inflammatory or a combination of both and take into account lifestyle habits, such as sun exposure and the healing process.




